The Lowdown on Fungal Acne: How to Identify and Treat It

Table of Contents:
- What is Fungal Acne, And How Does It Differ From Normal Acne?
- What Does Fungal Acne Look Like?
- What Are the Causes of Fungal Acne?
- Who Is More Likely to Have Fungal Acne?
- How Do You Treat Fungal Acne?
- How Can You Prevent Fungal Acne?
- When Should You See a Doctor?
- Conclusion
Fungal acne, or pityrosporum folliculitis, is a common skin condition that appears as clusters of small pimples and red, itchy bumps. You might be surprised to learn, though, that fungal acne is not acne! It is, in fact, one of many types of folliculitis, or an infection in your hair follicles.
In this article, we will go through everything you need to know about fungal acne, including causes, symptoms, and common treatments for this easy-to-solve but very uncomfortable condition.
What is Fungal Acne, And How Does It Differ From Normal Acne?
The first thing we need to reiterate is that fungal acne is not acne (or acne vulgaris) but rather a type of folliculitis or infection of your hair follicles.
In regular acne, excessive production of sebum and oil buildup leads to blockage of follicle passage resulting in bacterial growth. This causes the inflammation that leads to acne.1,2 However, in fungal acne, the problem is a fungal infection (or yeast) in the hair follicle caused by the sudden or rapid growth of a fungus called Malassezia or Pityrosporum - which is also known to cause dandruff on the scalp.3,4
The difference between fungal acne and normal acne has to do with very distinct microbial activity modes. In other words, fungal acne follows a very different mechanistic pathway: Your hair follicle becomes inflamed, allowing germs into the area and causing an infection.
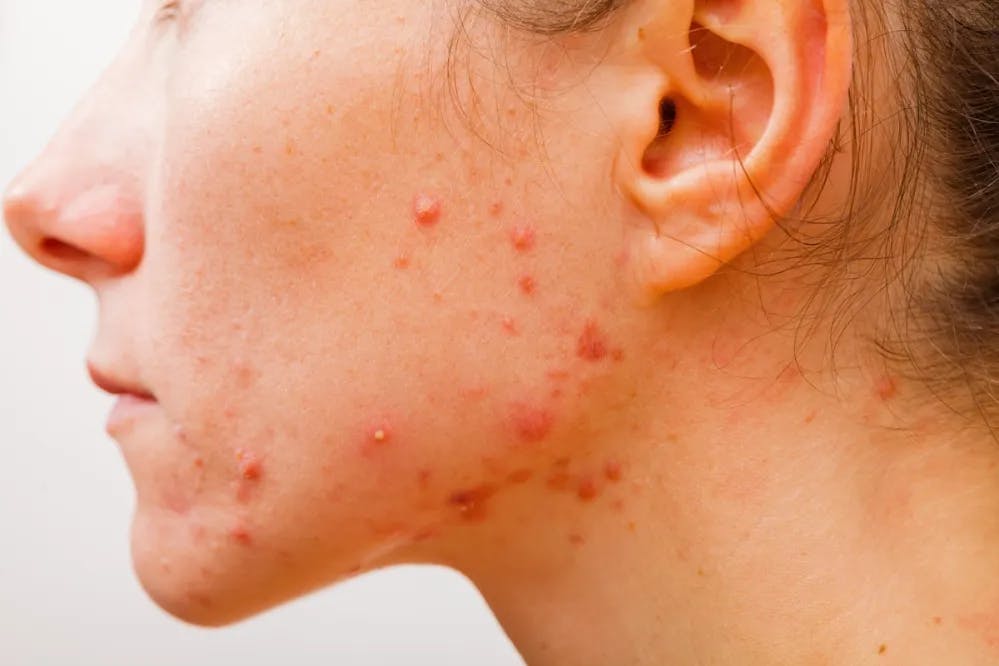
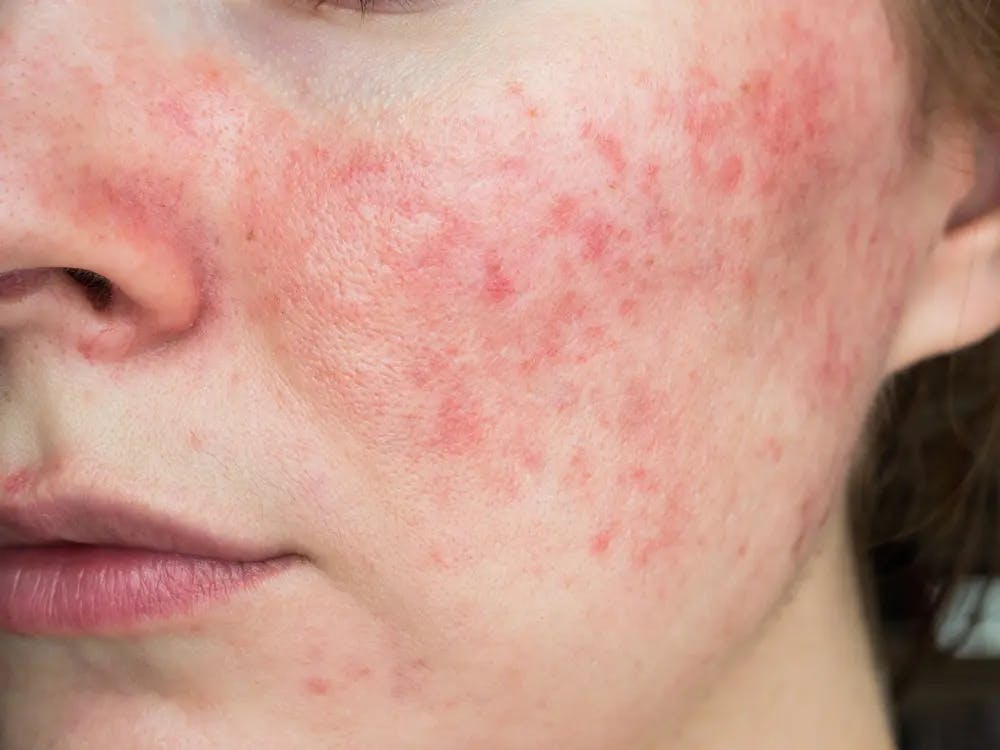
What Does Fungal Acne Look Like?
Fungal acne looks slightly different from normal acne. Mainly, this condition will appear as red bumps which are itchy (normal acne is usually not itchy) and, in more severe cases, may have pus.
These are the main symptoms of fungal acne or pityrosporum folliculitis:
- Clusters of small and red bumps.
- Very itchy skin (but no pain).
- Irritated hair follicles.
- Spots on the sides of your face, your forehead, and your chin.
- Spots on your back, neck, chest, and/or arms.
- Acne that doesn’t respond to treatment.
Keep in mind, though, that you might suffer from fungal acne and acne at the same time.
What Are the Causes of Fungal Acne?
In most cases, we can see a direct correlation between fungal acne and sweating. In fact, fungal acne is often a sign of poor hygiene.
Body parts with higher sweating are more vulnerable to this problem. The primary reason for this is that fungal acne (or abnormal growth of fungus over the skin) is an accumulation of sebum and sweat liquid - providing a good breeding ground for Malassezia fungi. Poor hygienic practices also facilitate fungal growth, so the cycle then continues.5
Scientific studies have also revealed relatively higher chances of fungus presence among teenagers. This is potentially due to hormonal changes in puberty age among adults.6
Other common causes of fungal acne include:
- Sweaty feet: When your skin is damp and hot, your hair follicles can become more easily damaged and irritated. For example, exercise can also increase the chances of developing pityrosporum folliculitis.
- Medication: Certain medications weaken your immune system, like oral corticosteroids, which can increase the chances of getting a fungal infection. Prolonged use of antibiotics can also disrupt the balance of bacteria and yeast present on your skin and lead to an overgrowth of both.
- A suppressed immune system: People with weakened immune systems, such as those undergoing chemotherapy or living with HIV/AIDS, are also at a higher risk of developing fungal acne.
- Diet: Certain foods (particularly dairy products and sugar) can promote the growth of yeast on your skin and exacerbate this skin condition.
- Clothes: Tight-fitting clothing (tight bras, athletic wear, etc.) can trap moisture against your skin and create a warm and humid environment where yeast can thrive - leading to fungal acne.
- Warm and wet environments: This problem can also be exacerbated in humid climates or during hot weather conditions, as they promote the growth of yeast.

Who Is More Likely to Have Fungal Acne?
Fungal acne, or pityrosporum folliculitis, can affect anyone. However, there are factors that increase a person’s risk of suffering from this skin condition.
Because fungal acne is more likely if you sweat a lot, sportspeople who do not take a shower after physical activity are particularly exposed. People with oily skin are also more prone, as oil provides a breeding ground for the yeast that causes fungal acne.
Abnormal hormonal activity as a result of medication or puberty can also lead to fungal infection and, as we covered in the section above, you will also be more vulnerable if you have a weakened or suppressed immune system, if you wear tight clothes, or if you have a diet high in sugar and dairy.
How Do You Treat Fungal Acne?
When talking about regular acne, the most popular treatments often target the bacteria that cause the issue. Unfortunately, most of those acne-focused activities will not be able to inhibit the growth of fungus.
For example, you can’t use regular anti-bacterial and anti-inflammatory formulations to treat fungal acne. Instead, you will need a product that has antifungal actives, such as zinc pyrithione, or sulfur. Both of these are known to have good antifungal activity and are commonly used in anti-dandruff formulations inhibiting the growth of Malassezia.
Likewise, ketoconazole and selenium sulfide are highly effective substances against fungus and are commonly available over the counter.
How Can You Prevent Fungal Acne?
The most common way to treat fungal acne is by using antifungal pills or topical creams and incorporating hygiene and self-care practices to help keep your skin healthy and clean. For example, changing your clothes right away after exercising or wearing looser clothing. You can also:
- Shower more regularly.
- Try a body wash.
- Use over-the-counter antifungal treatments.
- Try prescription oral antifungal medicine.
For mild cases, a topical antifungal medication (creams or lotions) might be enough to treat the problem. However, if the environment is right for the fungi to proliferate, lifestyle changes might not do the trick.
These OTC products can help treat fungal acne from the comfort of your home:
Rite Aid Clotrimazole Anti-fungal Cream
Rite Aid Clotrimazole Anti-fungal Cream is a potent treatment specifically formulated to combat fungal acne. It contains 1% clotrimazole, an antifungal agent that effectively targets the root cause of fungal infections, including fungal acne. This cream helps to alleviate symptoms, such as redness, inflammation, and breakouts caused by fungal overgrowth, promoting clearer and healthier skin.
Nizoral Anti-Dandruff Shampoo is a highly effective solution for combating fungal acne. With its active ingredient, ketoconazole, it possesses powerful antifungal properties that specifically target the overgrowth of fungi responsible for causing acne. To note, this is not a product specifically made for your face, proceed with caution when using this.
Additionally, there are also more common skincare ingredients that may aid in getting rid of fungal acne such as salicylic acid, zinc, benzoyl peroxide, and niacinamide.
Remember to do a patch test for any new products and introduce them gradually into your skincare routine. If your fungal acne persists or worsens, consult a dermatologist for further guidance and treatment options.
When Should You See a Doctor?
If you notice severe conditions (such as prolonged or significant outbreaks) and medical complications, you should always see a dermatologist. They will be able to prescribe an appropriate oral antifungal medication and recommend a maintenance treatment to keep the condition from reappearing.
Conclusion
Fungal acne (also referred to as pityrosporum folliculitis or malassezia folliculitis) is a form of folliculitis that occurs when yeast infects your hair follicles. This causes pimple-like bumps that are typically red, and itchy, and do not respond to normal acne treatments.
When it comes to fungal acne, prevention is key. There are several things you can do to try to avoid initiating or exacerbating the issue, such as wearing loose clothes made of breathable materials, always changing them right after you work out, and showering often.
If lifestyle changes don’t help, consider using OTC topical treatments containing ketoconazole, econazole nitrate, or clotrimazole.
For more skincare discussions, join us at Breakout!
References
- Downie, M.; Guy, R.; Kealey, T., Advances in sebaceous gland research: potential new approaches to acne management. Inter. J. of Cosmet. Sci 2004, 26 (6), 291-311.
- Bhate, K.; Williams, H., Epidemiology of acne vulgaris. British Journal of Dermatology 2013, 168 (3), 474-485.
- Ramasamy, S.; Barnard, E.; Dawson, T. L., Jr; Li, H., The role of the skin microbiota in acne pathophysiology. British Journal of Dermatology 2019, 181 (4), 691-699.
- Dawson Jr, T. L., The Role of the Scalp Microbiome in Health and Disease: Malassezia, Friend or Foe? J. Cosmet. Sci. 2021, 72, 634-642.
- Swaney, M. H.; Nelsen, A.; Sandstrom, S.; Kalan, L. R., Sweat and sebum preferences of the human skin microbiota. Microbiology Spectrum 2023, e04180-22.
- Park, J.; Schwardt, N. H.; Jo, J.-H.; Zhang, Z.; Pillai, V.; Phang, S.; Brady, S. M.; Portillo, J. A.; MacGibeny, M. A.; Liang, H., Shifts in the skin bacterial and fungal communities of healthy children transitioning through puberty. J. Invest. Dermatol. 2022, 142 (1), 212-219